High blood pressure, or hypertension, has been in the news recently. Hypertension has long been known to be a major risk factor for heart disease and stroke, so diagnosing and treating high blood pressure has always been important. A new report has changed the blood pressure classifications to reflect research suggesting that what was previously considered “too high” is really too high. Given the new report, this is a good time to review the diagnosis, health effects, and treatment of high blood pressure. This is the topic of my Health & Fitness column in the Aiken Standard this week.
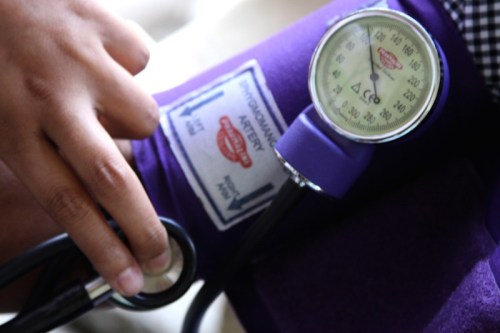
Hypertension is called the “silent killer” because it often has no symptoms but contributes to many heart attacks and strokes and is associated with type 2 diabetes, heart failure, and kidney disease. Since the risk of these conditions is related to the severity and how long your blood pressure has been high, blood pressure should be measured regularly.
The new guidelines lower the blood pressure at which more aggressive treatment is recommended for some patients who are at high risk for a heart attack or stroke. The guidelines also change the classifications of blood pressure, which may mean your doctor could start treatment sooner.
Know your numbers
Your blood pressure includes two numbers, both measured in millimeters of mercury (mmHg). The top number, systolic, is the pressure in your arteries while your heart is contracting and pumping blood. The bottom number is the diastolic pressure, which occurs between beats when the heart is relaxed. Both numbers are important.
According to the new guidelines, normal blood pressure is less than 120 mmHg systolic and less than 80 mmHg diastolic. If your blood pressure is between 120–129 mmHg systolic and 80–89 mmHg diastolic, you have elevated blood pressure. Stage 1 hypertension is 130–139 mmHg systolic or 80–89 mmHg diastolic and stage 2 hypertension is a blood pressure 140/90 and higher.
What is now called elevated BP and stage 1 hypertension used to be called “prehypertension.” The new classification should draw attention to the fact that the blood pressure is too high and prompt doctors and patients to begin treatment.
Get it down
If your blood pressure is above normal you should take treatment seriously. Lifestyle changes including eating a healthy diet, regular physical activity, weight control, and quitting smoking are all effective and essential for lowering blood pressure.
There are also many effective (and affordable) medications that your doctor can prescribe to lower your blood pressure. Take them as directed and don’t forget that they are designed to work with healthy lifestyle habits.
Keep it down
The aim, of course, isn’t simply to reduce your blood pressure using medications. Your ultimate goal should be to keep your blood pressure low without relying on medications, all of which have at least some negative side effects.
The best way to maintain a normal blood pressure is through daily exercise, eating a healthy diet, losing weight if you are overweight, and quitting smoking. A good place to start is the DASH diet, which is high in fruits, vegetables, and fiber and low in sodium and added sugar. The DASH diet has been shown to modestly lower blood pressure and lead to weight loss.
Since blood pressure tends to increase with age, even if you have normal blood pressure now you should take steps to prevent high blood pressure in the future. Adopting a lifestyle that includes daily physical activity, healthy eating habits, managing stress, and not smoking is essential for preventing high blood pressure. Additionally, these same health habits will help you prevent most other chronic disease including diabetes, heart disease, and many cancers.





